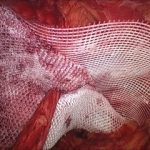
An inguinal hernia is an external protrusion of intra-abdominal contents through a natural weakness in this area, called the inguinal canal.
It occurs more commonly in men as the inguinal canal is wider, containing the spermatic cord structures. About 95% of all groin hernias diagnosed are inguinal in aetiology. Clinically, it appears as a bulge (or lump) in the groin on either side of the pubic bone, sometimes extending down to the scrotum.
Treatment options
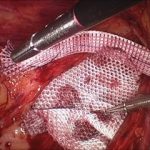
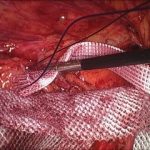
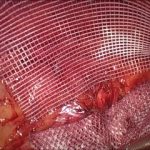
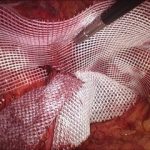
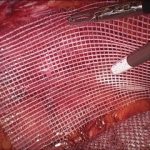
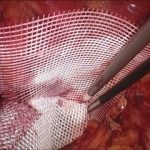
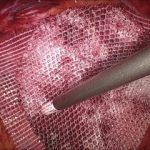
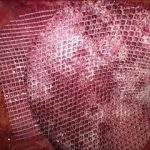
At the National Hernia Institute minimally invasive laparoscopic (keyhole) approach is the treatment of choice in which a camera is inserted into the layers of the abdominal wall through a small (10mm) incision. The laparoscope is a small fibreoptic viewing instrument that contains a lens, light source and video camera. The procedure is performed making three small incisions over the abdomen that will allow safe introduction of the laparoscopic instruments under direct vision, reduction of the hernia content and repair of the groin defect with insertion of a soft sheet of mesh.
In our Institute, we exclusively fix the mesh with biological fibrin glue as it is absolutely non-traumatic for the muscle, compared to the penetrating tackers or staples that most of the surgeons still routinely use. For instance, the risk of nerve or vessel injury is inexistent with fibrin glue. Prof Berney has 20-years expertise of fibrin glue usage for inguinal hernia repair, which represents the world largest collection of patients treated this way in a single Hernia Centre.
What are the benefits of laparoscopic inguinal hernia repair compared to open approach?
- Approach of choice for patients with bilateral (both sides) groin hernias
- Approach of choice for recurrent hernia following previous open repair
- Unique advantage of simultaneously treating any associated hernia (femoral, obturator) incidentally found during surgery. This is particularly relevant in women.
- Reduced severity of post-operative pain
- Reduced risk of developing chronic groin pain
- Faster return to normal professional and sport activities
- Reduced risk of mesh or groin infection
- Minimal scarring (smaller incisions)
- Reduced risk of hernia recurrence (only if performed in high-volume centres)
Causes
Some inguinal hernias have no apparent cause. Others might occur as a result of:
- Increased pressure within the abdomen
- A pre-existing weak spot in the abdominal wall
- Straining during bowel movements or urination
- Strenuous activity
- Pregnancy
- Chronic coughing or sneezing
In many people, the abdominal wall weakness that leads to an inguinal hernia occurs at birth when the abdominal lining (peritoneum) doesn’t close properly. Other inguinal hernias develop later in life when muscles weaken or deteriorate due to aging, strenuous physical activity or coughing that accompanies smoking.
Weaknesses can also occur in the abdominal wall later in life, especially after an injury or abdominal surgery.
In men, the weak spot usually occurs in the inguinal canal, where the spermatic cord enters the scrotum. In women, the inguinal canal carries a ligament that helps hold the uterus in place, and hernias sometimes occur where connective tissue from the uterus attaches to tissue surrounding the pubic bone.
Risk factors
Factors that contribute to developing an inguinal hernia include:
- Being male. Men are eight times more likely to develop an inguinal hernia than are women.
- Being older. Muscles weaken as you age.
- Being white.
- Family history. You have a close relative, such as a parent or sibling, who has the condition.
- Chronic cough, such as from smoking.
- Chronic constipation. Constipation causes straining during bowel movements.
- Pregnancy. Being pregnant can weaken the abdominal muscles and cause increased pressure inside your abdomen.
- Premature birth and low birth weight.
- Previous inguinal hernia or hernia repair. Even if your previous hernia occurred in childhood, you’re at higher risk of developing another inguinal hernia.
Wish to book an appointment or looking for some more information about our services,
get in touch and we will be happy to assist.