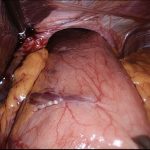
A hiatal hernia is a condition where part of the stomach that normally resides within the abdominal cavity slides through the diaphragm into the chest.
A hiatal hernia is a condition where part of the stomach that normally resides within the abdominal cavity slides through the diaphragm into the chest. With time, this hernia will progressively increase in size causing debilitating symptoms such as severe reflux (“heartburn”), difficulty swallowing or even breathlessness when most of the stomach has migrated into the chest. In our institution, gastroscopy and chest CT-scan are the two investigations of choice. On few occasions, specific testing to assess severity of reflux and contraction of the oesophagous (24-hours pH monitoring, manometry) might be required.

Conservative management
Conservative management is the initial step prior to considering surgical repair of hiatal hernia. This includes lifestyle changes:
- Losing or maintaining a healthy weight
- Bowel movement control (in case of chronic constipation)
- Avoiding food that may trigger heartburn (fatty or fried food, garlic, onion, caffeine, chocolate, mint, tomato sauce)
- Avoid smoking and alcohol intake
- Eating several smaller portion meals through the day (rather than a few large meals)
- Eating dinner at least 3-4 hours before going to bed
- Head elevation at night with pillows (about 15cm) while sleeping
- Start an antacid regimen with over the counter remedies
Treatment options
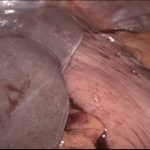
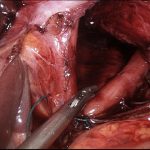
When those symptoms cannot be controlled despite lifestyle changes and appropriate medication, surgical treatment should be discussed. The hiatal hernia repair is almost exclusively performed using a minimally invasive laparoscopic (keyhole) approach.
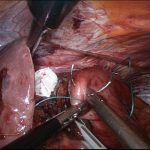
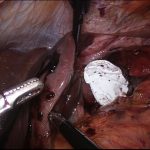
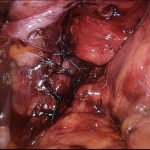
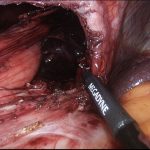
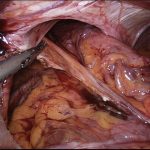
The stomach is completely reduced, the hernia sac excised, and the defect closed (cruroplasty). If the gap in the diaphragm is too large (closure under tension) or if the tissues are very weak, the repair will be reinforced with placement of a soft mesh that is fixed using fibrin glue. Use of tackers to fix the mesh is contraindicated due to the risk of major complications.
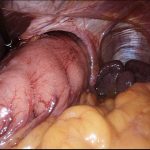
This mesh will be totally reabsorbed with 18 months and replaced by healthy scarring tissue, thus significantly reducing the potential risk of local damage to the lower oesophagous. Once completed, a partial fundoplication (stomach wrapped around the lower oesophagous) is created for better control of the reflux symptoms.
After being discharged home and while waiting for the swelling from surgery to settle down, a puree diet is generally maintained for 2 weeks, before progressively introducing normal food. Caution should be taken with bread, sticky rice, red meat and fizzy drinks. Heavy lifting or any strenuous activities should be avoided for 6-8 weeks.
Wish to book an appointment or looking for some more information about our services,
get in touch and we will be happy to assist.